This list is current as of January 2018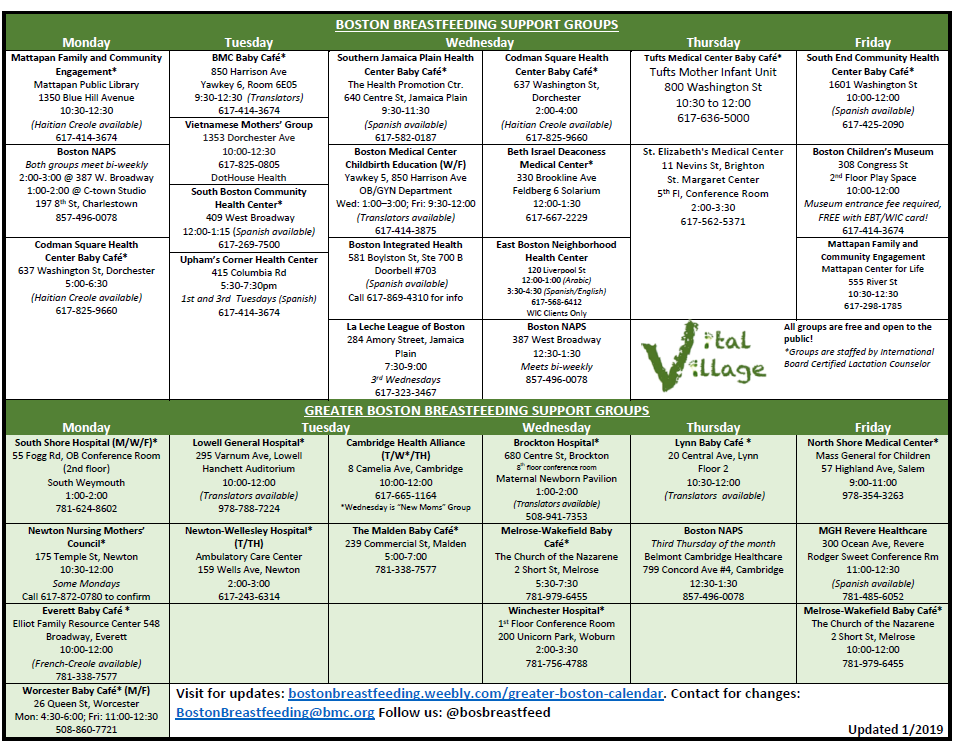
Five Ways to Grow Your (Doula) Business Without Social Media
In 2011, I made a bold move. About a year after attending my first birth, I decided to quit Facebook. To this day, I’m one of the only self-employed millennials I know who does not have a Bachelor’s degree or Facebook account. I’ve lived in the Boston area this whole time, so my list is specific to things I’ve found helpful to building a practice around home. Many new or aspiring birth doulas reach out to me to gain a better understanding of how to get into self-sustaining practice. Here are five things I’ve found especially helpful in building my practice, without the surveillance and privacy issues of using social media websites.
- Networking events. This may be most helpful to newer birth workers in order to get out there, meet expecting families, and get practice quickly answering questions like, “What is your philosophy?” “Why did you decide to become a doula?” and “Can you describe how your style differs from others?” Local to Boston, both Mama & Me in Jamaica Plain and OmBirths via Down Under Yoga have “Meet the Doulas” nights that are free for parents (often drawing a large crowd) and $20-$25 for a doula to sign up. It’s valuable to meet folks who may potentially want to hire you, but also to meet other birth workers in the area who may have different skillsets or might be available as backup.
- Grow your referral network. In order to be an asset to your community, you need to know what resources exist in your area that serve the folks you hope to work with. MassBirth is a good place to get started. They have lists of everything from placenta encapsulation to postpartum and lactation support, to mental health counselors.
- Know other people who have your dream job? Invite them to tea. Take the fifty minutes you may spend on Facebook in a day, and actually get together with someone who does related work in your area. Getting to know folks on a more personal level makes for a strong network of backup support and will likely get you more referrals in the future.
- MassDoulas yahoo group. Created and moderated by the lovely home birth midwife Joyce Kimball, MassDoulas is a place where local birth workers are constantly sharing information, events, clients looking for support.
- Volunteer. Yes, birth work is often under-compensated and if you’re called to attend births professionally, you should be well supported in order to make it a sustainable adventure. That being said, if you’re new to birth and nervous to claim Professional Doula Status with confidence, Brigham and Women’s Hospital offers a volunteer birth doula program for teen moms, and you don’t need to be certified in order to attend. It’s a great way to get an idea of what local hospital policies and practices are, and informs work you’ll do with clients for years to come. Even if you don’t have the capacity to volunteer for birth support directly, you could spend time lobbying for initiatives like the Massachusetts bill to cover doulas on MassHealth.
Herbalism and Herbal Resources
Herbalism and Herbalists
Local gem Bellx of Semilla of Ixchel offers full-spectrum reproductive support, herbal wisdom and customized preparations, and herbalism apprenticeships for People of Color in greater Boston. Offerings include an herbal CSA, placenta medicine, and workshops about holistic healing.
Muddy River Herbals is the project of Jenny Hauf and her husband Matt. They grow and wildcraft local, organic herbs for folks in the Boston area, and can be found at the Roslindale and Melrose Farmers Markets. Much of the calendula in my postpartum sitz baths comes from these guys!
While not local to the northeast, La Loba Loca is an incredible herbalist and friend who offers consultations, workshops, skillshares, knowledge shares, and seedlingships.
Clair Moore is a clinically trained herbalist and professional private chef who provides medicinal food preparation services around Boston, especially allergen-free foods for folks with autoimmune diseases or chronic illnesses. She and Amanda of The Willow Witch have also teamed up to create Willow Provisions, a medicinal herbal food supper club.
Herbstalk is a growing community of herbal classes in the Boston area. Based in Somerville, this yearly conference brings together folks from many herbal traditions every June.
Founded by Katja Swift and Ryn Midura, the CommonWealth Center for Holistic Herbalism in Brookline offers classes, apprenticeships and a clinic for low-income folks who seek herbal care.
Tammi Sweet at the Heartstone Center for Earth Essentials teaches an AMAZING anatomy & physiology class for holistically-minded folks who would otherwise shy away from a science-heavy class. She frequently offers free webinars on a variety of topics from allergies and asthma to the endocannabinoid system.
Abortion and Pregnancy Loss Resources
Abortion and Loss
The Boston Abortion Support Collective provides completely free support for people experiencing abortion, miscarriage or stillbirth in the Boston area. We have a small availability of affordable birth doulas, as well!
Backline is a judgement-free resource for folks considering what to do when they find themselves pregnant. They have a free phone line to discuss pregnancy options, and counseling before and after any decisions are made. Backline also started the resource Faith Aloud, in which clergy from various faith traditions are available to non-judgmentally counsel callers through decision making around pregnancy.
The Eastern Massachusetts Abortion Fund provides small grants to folks who need to access abortion care in Eastern Massachusetts in order to make abortion care more affordable.
The Pregnancy Panic Companion is a teen friendly resource for accurate information about pregnancy scares and available options.
Holding Our Space is an interactive community based around supporting those who have lost a pregnancy in any way. Stories of infertility, miscarriage, abortion, adoption, stillbirth and more are all supported and welcomed.
Fatherhood Resources
Fatherhood
Diaper Lab offers a Becoming A Dad class series.
William James College in Newton, MA hosts a free support group for new dads.
The Fatherhood Project is based in Boston.
Transgender Dad Carving Path of Opportunities for Son, Future
Rad Dad blog, zine and book focuses on the overlaps of various identities with fatherhood.
Postpartum and Lactation Support
Postpartum and Lactation Support
Postpartum Progress and Postpartum Support International promote awareness, prevention and treatment of mental health issues related to childbearing in every country worldwide. They also have a Perinatal Mental Health Alliance for Women of Color
Rachel Hess is an experienced and LGBTQ-friendly postpartum doula who also hosts parenting groups around Jamaica Plain.
Sophie Davis is a dear friend and postpartum doula, serving areas surrounding Newton.
The Every Mother Project provides training & support to birth, postpartum, lactation, and women’s health professionals who work with women and families in the childbearing year in order to reduce barriers that women with perinatal emotional complications face when accessing care.
Jewish Family and Children’s Services Center for Early Relationship Support provides a multitude of free support for young families in the Boston area. You do not have to be Jewish to utilize their services. They have support groups, therapy, and experienced moms who visit new ones to help you get the hang of feeding and caring for your little ones.
One of my doula mentors, Maria Dolorico, started A Mom is Born as a doula business, and has branched out into life coaching, lactation consulting, and holding groups for new parents in downtown Boston. She also offers a free online support course for families on how to plan for the postpartum period.
Zip Milk is a search engine for lactation consultants (LCs) in your area by zip code.
LC Home Visits contains a list of Boston-area international board certified lactation consultants (IBCLCs). In Massachusetts, it is required for insurance to cover lactation support.
BFAR is a resource for folks who want to breastfeed but have had breast/chest or nipple surgery in the past. Whether someone has had a diagnostic surgery, implants or a reduction, this website contains information about increasing the best chances for a healthy milk supply.
Milk Junkies is the website of trans dad, Trevor MacDonald. Once famous for being barred from La Leche League meetings, he now leads them locally in Canada and continues to blog about queer parenthood.
A mini study (22 participants) on transmasculine folks, chestfeeding and gender identity.
Boston-area breastfeeding support groups:

Home Birth Resources
Home Birth
The Massachusetts Midwives Alliance is a professional trade organization created by and for a dynamic and diverse group of midwives. The MMA was founded to build cooperation among midwives, and to promote midwifery as a means of improving health care for women and their families. Their website has a map of local home birth midwives around Boston.
Emily Bowler and Molly Geisler are continuing their local midwifery partnership, Modern Mama Midwifery. They attend home births, provide doula support and offer childbirth education classes.
Birth and Beyond of Jamaica Plain hosts the Mass Midwives Alliance training classes, as well as childbirth education and other events for parents and professionals.
Sarafina Kennedy and Jessica Patrone are midwifery partners supporting families from Greater Boston through Cape Cod.
Susanna Mauzy of Nightingale Midwifery attends births around Greater Boston and also helps families with home conception support.
Cesarean Birth and VBAC Resources
Cesarean Birth and VBAC
VBAC Facts is an evidence-based resource for information about the safety, options and factors involved in having a vaginal birth after a cesarean.
Julie Brill at Well Pregnancy teaches a class specifically for parents who are having a planned cesarean birth. It is based on Peggy Huddleston’s program, “Prepare for Surgery, Heal Faster.” It is free for folks who are going to Emerson Hospital.
ICAN is the International Cesarean Awareness Network. ICAN is a nonprofit organization whose mission is to improve maternal-child health by preventing unnecessary cesarians through education, providing support for cesarean recovery, and promoting Vaginal Birth After Cesarean (VBAC). There is also a Boston chapter that has meetings in Arlington, MA.
Cesarean Rates is a resource for the most up-to-date statistics of cesarean sections at hospitals around the United States. Here are the Massachusetts statistics.
Doulas and Birth Resources
Jacqui Morton is a doula, writer and founder of Holding Our Space, a participatory project centered around healing from reproductive loss. She also backs me up for births.
Maria of That Darn Doula is one of my backups in the area. She currently apprentices with a local home birth midwifery practice, and has experience at all local hospitals as well. She also backs me up for placenta encapsulation!
Tuly Duprat is an experienced birth doula who I connected with at Mama and Me. She is based in Malden, and has excellent rebozo skills. Tuly also speaks Portuguese.
Teresa Vittorioso-Fortin is a birth doula who offers childbirth classes through her practice, Entera Doula. She frequents Mount Auburn Hospital and is also fluent in Spanish.
Sierra at All Bodies Birth is a local birth and postpartum doula who especially loves to support LGBTQ+ families.
Jen at Douladventure brings her public health background to her work as a birth and postpartum doula in Boston.
Birth Sanctuary Boston is a group working to create an out-of-hospital birth option for families in Dorchester and beyond. It’s not easy work, but stay tuned for updates from them.
Beantown Babies is the combined project of doulas Emily and Lindsay. This amazing community space in Roslindale offers many things to new and growing families. From meditation workshops with Sophie, to childbirth ed classes with Teresa and acupressure for labor workshops with Ece, Beantown Babies has offerings that can enrich and support the pregnancy and birthing journeys of many local families.
Spinning Babies is a resource for fetal positioning and how it can affect labor. Tips for daily exercises/movements for getting baby engaged in the pelvis, as well as supportive labor positions can be found online.
The Miles Circuit is another series of simple movements to gently move baby into optimal positions for labor and delivery.
Mama and Me in Jamaica Plain offers a wide range of prenatal, postpartum, and child development classes for families in the Boston area. They host a bimonthly “Meet the Doulas” event that I frequently attend.
Doula Match is a search engine for folks looking for birth or postpartum doula support. You can compare profiles, availability, skillsets and experience all on one site.
Fertility and Conception Resources
My current favorite podcast, Fertility Friday is an amazing resource with TONS of free information about body literacy and the fertility awareness method. She has interviews with many fertility professionals around the topics of endometriosis, PCOS, thyroid disorders, autoimmunity, diet and lifestyle.
The Fertility Awareness Center can be a great beginner-friendly resource for tracking fertility cycles and getting to know your own signs of fertility. They do use lots of gendered language throughout the site. There is this little note about how fertility awareness tracking isn’t only just for straight, monogamous cis-women.
Angela Bell is an acupuncturist in Cambridge whose entire practice focuses on supporting fertility, conception and pregnancy.
New Moon Acupuncture is my dear colleague Ece’s practice includes acupuncture, moxibustion, manual therapies, nutritional counseling and lifestyle recommendation. She is based in Watertown.
Fertile Ground is a queer-friendly nurse and midwife team who provide compassionate gynecological care, fertility consultations and inseminations in the Boston area.
Susanna Mauzy at Nightingale Midwifery offers a full-spectrum of home birth midwifery care. She also offers fertility counseling and at-home insemination support. Susanna also runs the local International Cesarian Awareness Network groups in Arlington, MA.
Birthing Beyond the Binary hosts queer-friendly conception and childbirth education workshops online. They also have workshops for providers on how to support queer families in their practices. Online groups for queer families can be found here, as well!
Maia Midwifery is the practice of west-coast midwife, Kristin Kali. She offers individualized fertility counseling online, and conception support in person in Seattle. Her practice is built around supporting the needs of the LGBTQ community, parents conceiving over age 35, and single parents. She shares an amazing resource list with examples of known donor contracts, and parenting agreements for families who have more than two parents.
Choice Moms Podcast has a large amount of discussions and information surrounding fertility, conception, building a family as a single parent, adoption, conception with donor sperm and many topics related to these.


